Begin Your Journey to Better Health
Regenerative Medicine
We focus on harnessing the body’s natural healing capabilities to repair and restore damaged tissues and organs.
Spinal Decompression
If you are suffering from lower back and neck pain, sciatica pain, or bulging discs, gentle spinal decompression may be the answer for you.
Physical Therapy
Physical Therapy helps restore function, improve mobility, relieve pain, and prevent or limit permanent physical disabilities.
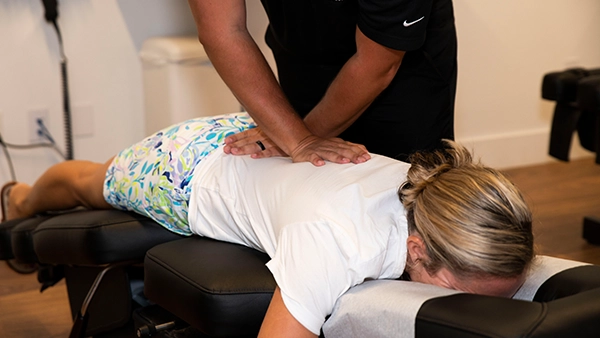
Chiropractic Care
Chiropractic adjustments are used to put your body back to its natural state, so that it may heal.
Weight Loss
We provide comprehensive solutions to help you achieve your weight management goals.
Medical Aesthetics
We specialize in enhancing your natural beauty and confidence through advanced non-surgical cosmetic procedures.

Chiropractor Coconut Creek FL
Welcome to our Integrated Health Center, where comprehensive healthcare meets accessibility. Our one-stop-shop approach offers a wide range of services to help you achieve and maintain long-term health. From chiropractic care to regenerative medicine and medical aesthetics, our team of physicians provides personalized care tailored to you. Using a mix of empathy, energy, and expertise, we strive to help educate and assist you with complicated health concepts. Rooted in trust, family, and growth, our Coconut Creek FL chiropractors are here to support you on your journey to health and vitality.

Request an Appointment
North Broward Wellness Center
We would like to express a warm welcome and genuine appreciation for trusting us with your health. At North Broward Wellness Center, your well-being is our top priority, and we’re committed to providing you with exceptional care, personalized attention, and a compassionate environment every step of the way.
Come visit our office and experience the difference for yourself. Say goodbye to ordinary healthcare and hello to a brighter, healthier future. Your journey to optimal wellness starts here – let’s make it amazing together!
Do You Suffer From Chronic Pain?
Most people believe that chiropractors treat back pain. That is true, but there is so much more that chiropractic care can achieve. Because chiropractors help to remove pressure from the nervous system, they can also influence many other conditions. It is common to hear chiropractic patients say that they came in for back pain and their headaches got better.
Chiropractic Explained
If you are looking for an explanation of how chiropractic care works this paragraph is for you. A concise scientific explanation of chiropractic is that adjustments directly affect muscle and bone structures by reducing pain and increasing joint motion.
That's a lot to take in, but it is the explanation as to why some chiropractic patients in Coconut Creek FL report improvement in body function. This is not a claim that chiropractic adjustments treat disease, but it does suggest that some people will see improvements in conditions that are outside of the treatment area.


The Education Of A Chiropractor
Most patients don't realize how much education chiropractors in Coconut Creek FL have. Chiropractors are held to some of the most intense educational standards in any health field. In fact, their education standards are very comparable to that of a medical doctor. After completing a strong emphasis of basic sciences in college, chiropractors attend a four-year chiropractic college. This means that chiropractors are primary care physicians. In other words, you don't have to have a referral to see a chiropractor.
Is chiropractic the right treatment for you? Call our team at North Broward Wellness Center in Coconut Creek FL. We will do our best to help you reach your goals.


Begin Your Journey to Health in 3 Easy Steps



